Rotator Cuff Tendonopathy
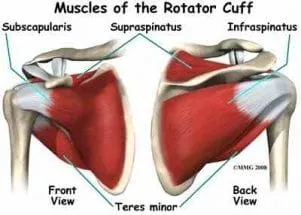
The rotator cuff includes four tendons: the supraspinatus, infraspinatus, teres minor and subscapularis as they insert into the capsule of the glenohumeral (ball and socket) joint. Collectively, the primary function of the rotator cuff is to stabilize the shoulder while the larger muscles move it. The supraspinatus muscle is also called upon to eccentrically decelerate an athlete’s arm after ball release, tennis serve, etc.
Rotator cuff injury is the most common problem to affect the shoulder, accounting for 4.5 million physician office visits per year (1). Injuries range from a mild strain of a single tendon to complete rupture of multiple tendons. Strains of the rotator cuff can occur abruptly from a single insult (falling, pushing, pulling, throwing or lifting) but more commonly ( over 90 percent) develop from multiple factors-including repetitive injury and age-related changes (2,3,4,31,33). Damage often begins and progresses from a partial to a full thickness tear (54,56,57). A “full thickness tear” is sometimes termed a “complete tear” and is not a rupture, but rather a hole or a slit in the tendon much like what would be created by running a knife lengthwise down the center of a rope. Most tears begin in the supraspinatus but may progress to involve the infraspinatus and subscapularis (3).
Risk factors:
The rotator cuff is predisposed to damage by a multitude of factors including obesity, high cholesterol, genetics or a history of corticosteroid injections (5-10). Impingement may produce recurring damage and impair the cuff’s ability to recover. Shoulder abduction (lifting arm above your head) is thought to impede blood flow by compressing or “wringing out” the critical zone. As we age, the natural vascularity of our tissue decreases while degenerative spurring increases, thereby advancing the age-related progression of degenerative cuff tendon failure (11). Smoking diminishes blood flow and is another known risk factor for the development of rotator cuff pathology. Research suggests that 95% of chronic rotator cuff tears are associated with impingement syndrome(32). Repetitive overhead activity predisposes a patient to impingement related injury- particularly sports like baseball, swimming, volleyball, tennis, rowing, weightlifting and archery and jobs including carpentry, painting, wallpaper hanging, cleaning windows and washing/ waxing cars. The unilateral nature of these tasks makes rotator cuff injury more common in the dominant arm (12). Patients with scapular dyskinesis or upper crossed syndrome are highly predisposed to rotator cuff damage from repetitive impingement.
Like tendinopathies affecting other areas of the body, the etiology of rotator cuff maladies is now considered more “degenerative” than “inflammatory”. It is a failed healing response (58-65).
Symptoms of rotator cuff injuries:
The clinical presentation for rotator cuff injury differs significantly between acute and chronic tears.
Acute tears:
Acute injuries, resulting from falls, throws or other powerful movements, begin as a “tearing” or “snapping” feeling accompanied by severe pain and weakness, particularly shoulder abduction.
Chronic tears:
Chronic or degenerative tears usually begin silently with widely variable symptoms, becoming more evident as the tear progresses (13). Patients often report gradual onset pain and weakness accompanied by clicking or noises in their shoulders. Pain may be localized to the anterolateral aspect of the shoulder but can radiate down the arm. Early symptoms are provoked by overhead activity and may progress to the point that the patient has difficulty raising their arm overhead. Pain is often worse at night, particularly when lying on the affected shoulder (36).
Signs of rotator cuff injury:
Shoulder range of motion testing will likely demonstrate limited passive internal rotation and decreased active elevation and abduction. (14-16) Slightly diminished internal rotation ROM on the patient’s dominant shoulder is common. Your doctor will also perform some orthopedic tests to determine if the rotator cuff is injured or aggravated.
Scapulohumeral rhythm:

Is imaging necessary for rotator cuff injuries?
The decisoin to image the shoulder (and all other imaging) should rely on whether the outcome of the study will affect treatment. Acute injury in a young patient suspected of having a rupture may warrant immediate advanced imaging, whereas an 80-year old patient with slow onset shoulder pain and weakness may not.
In cases where surgery is contemplated, both ultrasound and MRI are highly accurate (90%) in detecting complete rotator cuff tears (21,23, 79-82). MRI arthrography has long been considered the most sensitive test, particularly for detecting partial tears (34), however, it is not routinely recommended for diagnosing rotator cuff tears as it has a marginal benefit over plain MRI or Ultrasound (79). The likelihood of finding a rotator cuff tear on advanced imaging is relatively proportionate to the patient’s age. Researchers have shown that asymptomatic rotator cuff defects are present in 10% of those under the age of 20, 50% of people over 70 years of age, and 50-80% of people over 80 years of age (24,74,76,88). Not all tears are the source of the symptoms.
Treatment and management of rotator cuff injuries:
Although there is no consensus on the most appropriate management for rotator cuff injuries, current research suggests that conservative care should be the first choice for most non-traumatic tears (25, 45,75,76). The decision to initiate conservative versus surgical management should be based on acuity, tear size, age and loss of function (5). Data suggests that conservative management of partial thickness and chronic full-thickness tears yields good outcomes (5,28,29). Success rates for conservative care vary between 33-92%, and the prognosis seems to be based on the patient’s history, tear size and duration of symptoms (25). Findings from high-quality research investigations “suggest that a graduated and well-constructed exercise approach confers at least equivalent benefit as that derived from surgery for; subacromial pain (impingement) syndrome, rotator cuff tendinopathy, partial thickness rotator cuff (RC) tears and atraumatic full-thickness rotator cuff tears” (75).
*Long-term non-operative outcomes compare to surgical repairs (91).*
The conservative management of rotator cuff injuries should include activity modification, stretching, strengthening, manual therapy, and restoration of scapular mechanics (86). Patients should avoid painful overhead activity, carrying heavy objects and sleeping on the affected side, especially with the arm stretched overhead. Patients may benefit by sleeping on the unaffected side with a pillow between their affected arm and trunk. Smokers should consider a cessation program. Overweight patients would benefit from a diet and aerobic exercise regimen.
Treatment options:
Early interventions should minimize stressful loading of the injured tissues. Stretching and myofascial release techniques may be appropriate for the pectoral muscles, infraspinatus, teres minor, subscapularis, trapezius, levator and posterior capsule.
Transverse friction massage or IASTM may be implemented judiciously to enhance remodeling of scar tissue.
Low-level laser therapy may be helpful (86)
The use of elastic therapeutic tape may help to facilitate or inhibit muscular function.
Joint mobilization and manipulation are appropriate for restrictions in the scapulothoracic, glenohumeral joint, and cervicothoracic spine (30).
There is evidence to suggest that cervicothoracic and thoracic spine manipulation may help decrease shoulder pain while improving mobility and function (41-44,73).
Rotator cuff rehab should begin with moderate effort and low repetitions. Response to tensile loading may be assessed by the patient’s change in night pain. Increases in night pain indicate the current rehab load is excessive. Progression advances when the patient tolerates a given level of tensile load. (89).
Gentle range of motion exercises can begin with Codman pendulum exercises, wall walking and stick or towel exercises.
Stretching exercises should focus on restoring adduction, internal rotation, and external rotation. This may be accomplished by a cross body stretch and sleeper stretch.
Progressive resistance exercises can be implemented as tolerated for the rotator cuff and periscapular musculature, particularly the external rotators, serratus anterior and lower trapezius. Clinicians should correct deficits of hip mobility or trunk stability in throwers. Other treatment options:
The use of NSAIDs should be limited as these drugs inhibit collagen synthesis and may interfere with natural healing (71,72,79,83,84,85).
Although PRP injections have been shown promote tendon healing (68,69), existing literature does not support their use for rotator cuff tendinopathy. (56,70,71).
Patients who fail conservative therapy may have an orthopedic consultation.
Rotator cuff surgery patients who undergo concurrent biceps tendon repair demonstrate lower effectiveness. (87)
Arthroscopy patients demonstrate improved functional scores when a post-surgical sling is not utilized (92).
At Creekside Chiropractic & Performance Center, we are highly trained to treat this condition. We are the only inter-disciplinary clinic in Sheboygan county that provides chiropractic, myofascial release, ART (Active Release Technique), massage therapy, acupuncture, physiotherapy, rehabilitative exercise, nutritional counseling, personal training, and golf performance training under one roof. Utilizing these different services, we can help patients and clients reach the best outcomes and the best versions of themselves. Voted Best Chiropractor in Sheboygan by the Sheboygan Press.
Evidence Based-Patient Centered-Outcome Focused
Sources:
1. Oh LS, Wolf BR, Hall MP, Levy BA, Marx RG. Indications for rotator cuff repair: a systematic review. Clin Orthop Relat Res 2007;455:52-63
2. Kibler WB, Chandler TJ, Pace BK. Principles of rehabilitation after chronic tendon injuries. Clin
Sports Med 1992;11:661–73
3. Ozaki J, Fujimoto S, Nakagawa Y, Masuhara K, Tamai S. Tears of the rotator cuff of the shoulder associated with pathological changes in the acromion: a study in cadavers. J Bone Joint Surg Am 1988;70:1224-30
4. Kibler, WB. Rehabilitation of rotator cuff tendinopathy. Clin Sp Med. 2003;22(4):837-847.
5. Tashjian RZ Epidemiology, natural history, and indications for treatment of rotator cuff tears. Clin Sports Med. 2012 Oct;31(4):589-604.
6. Wendelboe AM, Hegmann KT, Gren LH, Alder SC, White GL Jr, Lyon JL. Associations between body-mass index and surgery for rotator cuff tendinitis. J Bone Joint Surg Am 2004;86:743-7.
7. Galatz LM, Silva MJ, Rothermich SY, Zaegel MA, Havlioglu N, Thomopoulos S. Nicotine delays tendon-to-bone healing in a rat shoulder model. J Bone Joint Surg Am 2006;88:2027-34
8. Wei AS, Callaci JJ, Juknelis D, et al. The effect of corticosteroid on collagen expression in injured rotator cuff tendon. J Bone Joint Surg Am 2006;88:1331-8.
9. Wiggins ME, Fadale PD, Ehrlich MG, Walsh WR. Effects of local injection of corticosteroids on the healing of ligaments: a follow-up report. J Bone Joint Surg Am 1995;77:1682-91.
10. Blair B, Rokito AS, Cuomo F, Jarolem K, Zuckerman JD. Efficacy of injections of corticosteroids for subacromial impingement syndrome. J Bone Joint Surg Am 1996;78:1685-9.
11. Yamaguchi K, Ditsios K, Middleton WD, Hildebolt CF, Galatz LM, Teefey SA. The demographic and morphological features of rotator cuff disease: a comparison of asymptomatic and symptomatic shoulders. J Bone Joint Surg Am 2006;88:1699-704
12. Yamamoto A et al. Prevalence and risk factors of a rotator cuff tear in the general population. Shoulder Elbow Surg. 2010 Jan;19(1):116-20.
13. Duckworth DG, Smith KL, Campbell B, Matsen FA III. Self-assessment questionnaires document substantial variability in the clinical expression of rotator cuff tears. J Shoulder Elbow Surg 1999;8:330-3
14. Putnam CA. Sequential motions of body segments in striking and throwing skills: Description and explanations. J Biomech 1993;26(suppl 1):125-135
15. Laudner KG, Myers JB, Pasquale MR, Bradley JP, Lephart SM. Scapular dysfunction in throwers with pathologic internal impingement. J Orthop Sport Phys Ther 2006; 36:485-494
16. Kibler WB, Sciascia AD, Thomas SJ. Glenohumeral internal rotation deficit: Pathogenesis and response to acute throwing. Sports Med Arthrosc 2012;20:34-38.
17. Jobe FW Maoynes DR Deleniation of diagnostic criteria and a rehabilitation program for rotator cuff injuries. Am J Sports Med 10:336-339 1982
18. Robb AJ, Fleisig G, Wilk K, Macrina L, Bolt B, Pajaczkowski J. Passive ranges of motion of the hips and their relationship with pitching biomechanics and ball velocity in professional baseball pitchers. Am J Sports Med 2010;38:2487-2493.
19. Toyoshima S, Hoshikawa T,MiyashitaM. Contributions of body parts to throwing performance. In: Biomechanics IV. Baltimore: University Park Press, 1974;169-174.
20. Murrell GA, Walton JR. Diagnosis of rotator cuff tears. The Lancet. 2001;357(9258):769-770
21. Teefey SA, Rubin DA, Middleton WD, Hildebolt CF, Leibold RA, Yamaguchi K. Detection and quantification of rotator cuff tears: comparison of ultrasonographic, magnetic resonance imaging, and arthroscopic findings in seventy-one consecutive cases. J Bone Joint Surg Am 2004;86:708-16
22. Neer
23. Iannotti JP, Ciccone J, Buss DD, et al. Accuracy of office-based ultrasonography of the shoulder for the diagnosis of rotator cuff tears. J Bone Joint Surg Am 2005;87:1305-11.
24. Milgrom C, Schaffler M, Gilbert S, van Holsbeeck M. Rotator-cuff changes in asymptomatic adults: the effect of age, hand dominance and gender. J Bone Joint Surg Br 1995;77:296-8
25. Longo UG et al. Conservative treatment and rotator cuff tear progression. Med Sport Sci. 2012;57:90-9.
27. Bartolozzi A, Andreychik D, Ahmad S: Determinants of outcome in the treatment of rotator cuff disease. Clin Orthop Relat Res 1994, 308:90-97.
28. Ainsworth R, Lewis JS. Exercise therapy for the conservative management of full thickness tears of the rotator cuff: clinical practice a systematic review. Br J Sports Med 2007;41:200-10
29. Baydar M et al. The efficacy of conservative treatment in patients with full-thickness rotator cuff tears. Rheumatol Int. 2009 Apr;29(6):623-8.
30. Manske RC, Meschke M, Porter A, Smith B, Reiman M. A randomized controlled single-blinded comparison of stretching versus stretching and joint mobilization for posterior shoulder tightness measured by internal rotation motion loss. Sports Health 010;2:94-100.
31. Thomas R, Berquist HMRI of the Musculoskeletal System 6th edition 2012, by Lippincott Williams & Wilkins
32. Neer CE III. Impingement lesions. Clin Orthop. 1983;173:70–77.
33. Zlatkin MB. MRI of the Shoulder. Philadelphia, PA: Lippincott Williams & Wilkins; 2003.
34. de Jesus JO, Parker L, Frangos AJ, et al. Accuracy of MRI, MR arthrography, and ultrasound in the diagnosis of rotator cuff tears: A meta-analysis. AJR Am J Roentgenol. 2009;192:1701–1707.
35. Beall DP, Williamson EE, Ly JQ, et al. Association of biceps tendon tears with rotator cuff abnormalities: degree of correlation with tears of the anterior and superior portions of the rotator cuff. AJR Am J Roentgenol. 2003;180:633–639.
36. Litaker D, Pioro M, El Bilbeisi H, Brems J. Returning to the bedside: using the history and physical exam to identify rotator cuff tears. J Am Geriatr Soc 2000;48:1633-7.
37. Hertel R, Ballmer RT, Lombert SM, Gerber C. Lag signs in the diagnosis of rotator cuff rupture. J Shoulder Elbow Surg 1996;5:307-13.
38. Itoi E, Kido T, Samo A, Urayama M, Sato K. Which is more useful, the “full can test” or the “empty can test,” in detecting the torn supraspinatus tendon? Am J Sports Med 1999;27:65-8.
39. Walch G, Boulahia A, Calderone S, Robinson AHN. The `dropping’ and hornblower’s’ signs in evaluation of rotator-cuff tears. J Bone Joint Surg Br 1998; 80:624-8.
40. Barth JR, Burkhart SS, De Beer JF. The bear-hug test: a new and sensitive test for diagnosing a subscapularis tear. Arthroscopy 2006; 22:1076-1084.
41. Crosbie J, Kilbreathe SL, Hooman L, York S. Scapulohumeral rhythm and associated spinal motion. Clin Biomechan. 2008; 23: 184-192.
42. Strunce JB, et al. The Immediate Effects of Thoracic Spine and Rib Manipulation on Subjects with Primary Complaints of Shoulder Pain J Man Manip Ther. 2009; 17(4): 230–236.
43. Walser RF, Meseve BB, Boucher TR. The Effectiveness of Thoracic Spine Manipulation for the Management of Musculoskeletal Conditions: A Systematice Review and Meta-Analysis of Randomized Controlled Trials. J Man Manip Ther. 2009; 17(4): 237-246.
44. Muth S et al. The Effects of Thoracic Spine Manipulation in Subjects With Signs of Rotator Cuff Tendinopathy Journal of Orthopaedic & Sports Physical Therapy, 2012, Volume: 42 Issue: 12 Pages: 1005-1016
45. Kukkonen J, Joukainen A, Lehtinen J, Mattila KT, Tuominen EK, Kauko T, Aärimaa V. Treatment of non-traumatic rotator cuff tears: A randomised controlled trial with one-year clinical results. Bone Joint J. 2014 Jan;96-B(1):75-81.
46. Littlewood C, Malliaras P, Mawson S, May S, Walters SJ. Self-managed loaded exercise versus usual physiotherapy treatment for rotator cuff tendinopathy: a pilot randomised controlled trial. Physiotherapy. 2014 Mar;100(1):54-60.
47. Hertel R, Ballmer FT, Lombert SM, Gerber C. Lag signs in the diagnosis of rotator cuff rupture. J Shoulder Elbow Surg. 1996;5:307–313.
48. Blonna D, Cecchetti S, Tellini A, et al. Contribution of the supraspinatus to the external rotator lag sign: kinematic and electromyographic pattern in an in vivo model. J Shoulder Elbow Surg. 2010;19:392–398.
49. Lohr JF, Uhthoff HK. The microvascular pattern of the supraspinatus tendon. Clin Orthop. 1990;254:35–38.
50. Goodmurphy CW, Osborn J, Akesson EJ, et al. An immunocytochemical analysis of torn rotator cuff tendon taken at the time of repair. J Shoulder Elbow Surg. 2003;12:368–374.
51. Brooks CH, Revell WJ, Heatley FW. A quantitative histological study of the vascularity of the rotator cuff tendon. J Bone Joint Surg Br. 1992;74:151–153.
52. Fukuda H, Hamada K, Yamanaka K. Pathology and pathogenesis of bursal-side rotator cuff tears viewed from en bloc histologic sections. Clin Orthop Relat Res. 1990;254:75–80.
53. Swiontkowski MF, Iannotti JP, Boulas HJ, Esterhai JL. Intraoperative assessment of rotator cuff vascularity using laser Doppler flowmetry. In: Post M, Morrey BF, Hawkins RJ, editors. Surgery of the shoulder. St. Louis: Mosby-Year Book; 1990.
54. Ogata S, Uhthoff HK. Acromial enthesopathy and rotator cuff tear. A radiologic and postmortem investigation of the coracoacromial arch. Clin Orthop. 1990;254:39–48.
55. Budoff EF, Rodin D, Ochiai D, Nirschl RP. Arthroscopic Rotator Cuff Debridement Without Decompression for the Treatment of Tendinosis. Arthroscopy: The Journal of Arthroscopic and Related Surgery. 2005;21:1081–1089
56. Vai AG, Cupis MD, et al. Clinical and Biological Aspects of Rotator Cuff Tears. Muscles Ligaments Tendons J. 2013 February 24; 3(4): 359.
57. H. Mike Kim et al. Location and Initiation of Degenerative Rotator Cuff Tears An Analysis of Three Hundred and Sixty Shoulders J Bone Joint Surg Am. 2010 May; 92(5): 1088–1096.
58. Codman EA. The shoulder. Boston: Thomas Todd; 1934. Rupture of the supraspinatus tendon; pp. 123–177.
59. Hashimoto T, Nobuhara K, Hamada T. Pathologic evidence of degeneration as a primary cause of rotator cuff tear. Clin Orthop Relat Res. 2003;415:111–120.
60. Ozaki J, Fujimoto S, Nakagawa Y, et al. Tears of the rotator cuff of the shoulder associated with pathological changes in the acromion: a study in cadavera. J Bone Joint Surg Am. 1998;70:1224–1230.
61. Yuan J, Murrell GA, Wei AQ, Wang MX. Apoptosis in rotator cuff tendinopathy. J Orthop Res. 2002;20:1372–1379.
62. Yadav H, Nho S, Romeo A, MacGillivray JD. Rotator cuff tears: pathology and repair. Knee Surg Sports Traumatol Arthrosc. 2009;17:409–421. 57.
63. Nirschl RP. Rotator cuff tendinitis: Basic concepts of pathoetiology. Instr Course Lect. 1989;38:439–445.
64. Khan K, Cook J. The painful nonruptured tendon: Clinical aspects. Clin Sports Med. 2003;22:711–725.
65. Ishii H, Brunet JA, Welsh RP, et al. “Bursal reactions” in rotator cuff tearing, the impingement syndrome, and calcifying tendonitis. J Shoulder Elbow Surg. 1997;6:131–136.
66. Lin TW, Cardenas L, Soslowsky LJ. Biomechanics of tendon injury and repair. J Biomech. 2004;37:865–877.
67. Murrell GA, Lilly EG, III, Goldner RD, Seaber AV, Best TM. Effects of immobilization on achilles tendon healing in a rat model. Journal of Orthopaedic Research. 1994;12:582–591.
68. De Mos M, van der Windt AE, Jahr H, et al. Can platelet-rich plasma enhance tendon repair? A cell culture study. Am J Sports Med. 2008;36:1171–1178.
69. Mishra A, Woodall J, Jr, Vieira A. Treatment of tendon and muscle using platelet-rich plasma. Clin Sports Med. 2009;28:113–125.
70. Randelli PS, Arrigoni P, Ragone V, Aliprandi A, Cabitza P. Platelet rich plasma in arthroscopic rotator cuff repair: a prospective RCT study, 2-year follow-up. J Shoulder Elbow Surg. 2011;20:518–528.
71. Al-Sady O, Schulze-Tanzil G, Kohl B, et al. Tenocytes, pro-inflammatory cytokines and leukocytes: a relationship? MLTJ. 2011;1:68–76.
72. Del Buono A, Oliva F, Osti L, Maffulli N. Metalloproteases and tendinopathy. MLTJ. 2013;3(1):51–57.
73. Southerst D, Yu H, Randhawa K, Côté P, D'Angelo K, Shearer HM, Wong JJ, Sutton D, Varatharajan S, Goldgrub R, Dion S, Cox J, Menta R, Brown CK, Stern PJ, Stupar M, Carroll LJ, Taylor-Vaisey A. Chiropr Man Therap. 2015 Oct 27;23:30. The effectiveness of manual therapy for the management of musculoskeletal disorders of the upper and lower extremities: a systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Chiropractic & Manual Therapies (2015) 23:30
74. Teunis, Teun et al. A systematic review and pooled analysis of the prevalence of rotator cuff disease with increasing age. Journal of Shoulder and Elbow Surgery , Volume 23 , Issue 12 , 1913 – 1921
75. Lewis J. Rotator cuff related shoulder pain: Assessment, management and uncertainties. Man Ther. 2016 Jun;23:57-68.
76. Edwards P,et al. Exercise rehabilitation in the non-operative management of rotator cuff tears: A review of the literature. Int J Sports Phys Ther. 2016 Apr;11(2):279-301.
77. Castoldi F. et al. External rotation lag sign revisited: accuracy for diagnosis of full thickness supraspinatus tear. Journal of Shoulder and Elbow Surgery. 2009 Jul-Aug;18(4):529-34.
78. Jain NB, et al. The Diagnostic Accuracy of Special Tests for Rotator Cuff Tear: The ROW Cohort Study. Am J Phys Med Rehabil 96 (3), 176-183. 3 2017.
79. Tuite MJ, et al. Imaging Evaluation of Nonacute Shoulder Pain. AJR Am J Roentgenol. 2017 May 24:1-9. doi: 10.2214/AJR.17.18085. [Epub ahead of print]
80. Dinnes J, Loveman E, McIntyre L, Waugh N. The effectiveness of diagnostic tests for the assessment of shoulder pain due to soft tissue disorders: a systematic review. Health Technol Assess 2003; 7:1–166
81. de Jesus JO, Parker L, Frangos AJ, Nazarian LN. Accuracy of MRI, MR arthrography, and ultra-sound in the diagnosis of rotator cuff tears: a meta-analysis. AJR 2009; 192:1701–1707
82. Lenza M, Buchbinder R, Takwoingi Y, Johnston RV, Hanchard NC, Faloppa F. Magnetic resonance imaging, magnetic resonance arthrography and ultrasonography for assessing rotator cuff tears in people with shoulder pain for whom surgery is being considered. Cochrane Database Syst Rev 2013; 9:CD009020
83. Mackey AL, Mikkelsen UR, Magnusson SP, Kjaer M. Rehabilitation of muscle after injury—the role of anti-inflammatory drugs. Scand J Med Sci Sports. 2012;22(4):e8–e14.
84. Mendias CL, Tatsumi R, Allen RE. Role of cyclooxygen-ase-1 and -2 in satellite cell proliferation, differentiation, and fusion. Muscle Nerve. 2004;30(4):497–500.
85. Shen W, Li Y, Tang Y, Cummins J, Huard J. NS-398, a cyclooxygenase-2-specific inhibitor, delays skeletal muscle healing by decreasing regeneration and promoting fibrosis. Am J Pathol. 2005;167(4):1105–1117.
86. Hawk C. Systematic Review of Nondrug, Nonsurgical Treatment of Shoulder Conditions. J Manipulative Physiol Ther 2017 Jun ;40(5):293-319
87. Gialanella B, Grossetti F, Mazza M, Danna L, Comini L. Functional Recovery After Rotator Cuff Repair: The Role of Biceps Surgery. J Sport Rehabil. 2018 Jan 1;27(1):83-93
88. Guffey JS, et al. Degenerative Changes in Asymptomatic Subjects: A Descriptive Study Examining the Using Musculoskeletal Sonography in a Young Population.
J Allied Health. 2018.
89. Cook JL, Purdam CR. The challenge of managing tendinopathy in competing athletes. Br J Sports Med. 2014;48:506-509.
90. Almekinders LC, Weinhold PS, Maffulli N. Compression etiology in tendinopathy. Clin Sports Med. 2003;22:703-710.
91. Boorman RS, More KD, Hollinshead RM, et al. What happens to patients when we do not repair their cuff tears? Five-year rotator cuff quality-of-life index outcomes following nonoperative treatment of patients with full-thickness rotator cuff tears. J Shoulder Elbow Surg. 2018;27(3):444-448.
92. Tirefort J et al. Postoperative Mobilization After Superior Rotator Cuff Repair: Sling Versus No Sling: A Randomized Prospective Study. J Bone Joint Surg Am. 2019 Mar 20;101(6):494-503. doi: 10.2106/JBJS.18.00773.
