Cervical spine stenosis is narrowing of the central spinal canal or neural foramina due to changes in bone or soft tissue. Stenotic compression may involve one nerve root, multiple nerve roots or most significantly, the spinal cord (myelopathy). Cervical spine stenosis is present in almost 5% of the adult population (1). The condition shows age-related progression, affecting nearly 7 percent of those over 50, and 9 percent of those over 70 (1).
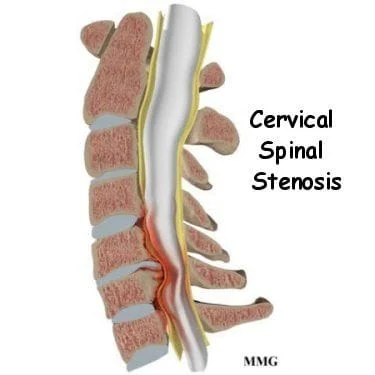
Stenosis may develop from multiple factors, and it is often a combination of those factors that grow to reach a critical level of compression. Stenosis may be "congenital" or may be "acquired". The most common cause of stenosis is degenerative changes (2). In the normal aging process of the spine, the discs thin and spreads circumferentially. This places extra load on the many joints surrounding the discs. This generates pain and decreased range of motion, which is then followed by degeneration. Osteophytes ("bone spurs") can develop on the around the joints due to the increased stress (Wolff's law).
What are the symptoms of cervical spinal stenosis?
The natural history of stenosis is typically a slow, steady progression, although some patients' symptoms remain stable or even improve over time (5,12,27). Symptoms correspond to the progression degeneration and advance from local arthritic pain to radicular pain. Initially, neck pain and headaches are common. Symptoms may refer into the shoulder, arm, and upper back. Nerve root compression can cause radicular complaints of pain, pins and needles, tingling, or weakness in the shoulders, arms, or hands. Eventually, progressive cord compression causes loss of fine motor skills of the hand (perceived as clumsiness), leg pain, paresthesia, numbness, weakness, gait and balance disturbances, difficulty walking, and possible loss of bowel or bladder control. Patients who have progressed to myelopathy report relatively little to no neck pain.
Are x-rays or other imaging needed for cervical spinal stenosis?
Radiographic imaging is essential to define stenosis (28). The normal sagittal diameter of the spinal canal, as measured on lateral radiographs, is approximately 17-18 mm (10). “Relative stenosis” is defined as having a canal between 10-13 mm, with “absolute stenosis” in canals measuring less than 10 mm. Flexion/extension views that demonstrate greater than 3 mm of translation suggest instability as a possible contributor. MRI is the preferred method of diagnostic imaging for stenosis, as it can see both hard and soft causes of encroachment (12,28).
What are the best treatment options for cervical spinal stenosis?
The need for neurosurgical consultation progresses proportionately with the course of stenosis. Any signs or symptoms of central cord compression warrant immediate neurosurgical evaluation. In the absence of myelopathy or significant nerve root involvement, a trial of conservative care may be prudent (16,24). Conservative treatments are directed at relieving symptoms and preserving cervical spine mobility and strength.
While patients with biomechanical joint dysfunction from early spondylosis may benefit tremendously from spinal manipulation, the presence of myelopathy is an absolute contraindication to HVLA manipulation (17). Low-force techniques, including Grade 1-4 mobilization, activator, and cervical flexion distraction may be more appropriate for patients with more than moderate degenerative change.
Nerve mobilization technique and cervical traction have been advocated in the treatment of stenosis patients (18,19) Nerve mobilization techniques may help reduce nerve adherence, facilitate nerve gliding, decrease mechanosensitivity, reduce intraneural swelling and improve axoplasmic flow (20,21). Cervical traction may result in pain inhibition, separation of vertebral bodies, neuroforaminal widening, and decreased intradiscal pressure (18,19, 22,23,31). Traction has shown to provide relief for cervical radicular complaints (32). Patients can be sent home with nerve mobilization exercises and instructed on the use of home traction (15-20 minutes, 2-3 times per day with a weight of 10 pounds slowly increasing toward 20).
Modalities including acupuncture, ice, heat, massage, ultrasound, and electrical stimulation may provide symptomatic relief. Soft tissue manipulation, IASTM, and contract/relax stretching may be used to address areas of myofascial involvement in the cervical and shoulder girdle musculature. Exercises may be implemented prudently to improve neck mobility and muscular strength as well as extremity coordination, balance, and aerobic capacity. Cervical strengthening exercises may assist with intersegmental stability.
Medical co-management may include NSAIDs and muscle relaxants. Epidural steroid injections may provide some benefit for radicular complaints, but their use for central canal stenosis is controversial. Neurosurgical consultation is appropriate for any patient with signs of stenosis and is a necessity in cases of myelopathy. Based upon the status and progression of the disease, a careful “wait and watch” approach to surgery may be appropriate. Surgical intervention is directed at relieving pressure on the spinal cord and nerve roots, often through decompressive laminectomy coupled with a spinal fusion (24,25).
At Creekside Chiropractic & Performance Center, we are highly trained to treat cervical spinal stenosis with conservative care, and we work together with orthopedists to ensure the best standard of care is given. We are the only inter-disciplinary clinic in Sheboygan county that provides chiropractic, myofascial release, ART (Active Release Technique), massage therapy, acupuncture, physiotherapy, rehabilitative exercise, nutritional counseling, personal training, and golf performance training under one roof. Utilizing these different services, we can help patients and clients reach the best outcomes and the best versions of themselves. Voted Best Chiropractor in Sheboygan by the Sheboygan Press.
Evidence Based-Patient Centered-Outcome Focused
Sources:
1. Lee MJ, Cassinelli EH, Riew KD. Prevalence of cervical spine stenosis: anatomic study in cadavers. JBJS. 2007 Feb 1;89(2):376-80. Link
2. Montgomery DM, Brower RS. Cervical spondylotic myelopathy. Clinical syndrome and natural history. The Orthopedic Clinics of North America. 1992 Jul;23(3):487-93. Link
3. Carette S, Fehlings MG. Cervical radiculopathy. New England Journal of Medicine. 2005 Jul 28;353(4):392-9. Link
5. Kada?ka Z, Bedna?ík J, Novotný O, Urbánek I, Dušek L. Cervical spondylotic myelopathy: conservative versus surgical treatment after 10 years. European Spine Journal. 2011 Sep 1;20(9):1533-8. Link
6. Hai-bin C, Zheng-guo W, Ling Z, Yi W, Jing-cheng L, Li-ying Z, Min D, Shuang-ming S. Cervical spinal canal narrowing and cervical neurological injuries. Chinese Journal of Traumatology. 2012 Feb 1;15(1):36-41. Link
8. Shabat S, Leitner Y, David R, Folman Y. The correlation between Spurling test and imaging studies in detecting cervical radiculopathy. Journal of neuroimaging. 2012 Oct;22(4):375-8. Link
9. Young WF. Cervical spondylotic myelopathy: a common cause of spinal cord dysfunction in older persons. American family physician. 2000 Sep;62(5):1064-70. Link
10. Murone I. The importance of the sagittal diameters of the cervical spinal canal in relation to spondylosis and myelopathy. The Journal of bone and joint surgery. British volume. 1974 Feb;56(1):30-6. Link
11. Torg J. Relationship of cervical canal narrowing. Cervical Spine Research Society, New Orleans. 1989.
12. Thomé C, Börm W, Meyer F. Degenerative lumbar spinal stenosis: current strategies in diagnosis and treatment. Deutsches Ärzteblatt international. 2008 May;105(20):373. Link
13. Kang Y, Lee JW, Koh YH, Hur S, Kim SJ, Chai JW, Kang HS. New MRI grading system for the cervical canal stenosis. American Journal of Roentgenology. 2011 Jul;197(1):W134-40. Link
14. Baron EM, Young WF. Cervical spondylotic myelopathy: a brief review of its pathophysiology, clinical course, and diagnosis. Neurosurgery. 2007 Jan 1;60(suppl_1):S1-35. Link
15. Dawson DM, Potts F. Acute nontraumatic myelopathies. Neurologic clinics. 1991 Aug 1;9(3):585-603. Link
16. Nakamura, et al. Conservative treatment of CSM. J of Spinal Disorders 1998;11(2):175-179.
17. Bertelsman TJ, Indications and Contraindications to Spinal Manipulation: A review of the Literature. Presentation, American Back Society Meetings, San Francisco, CA December, 1995
18. Yang JD, Tam KW, Huang TW, Huang SW, Liou TH, Chen HC. Intermittent cervical traction for treating neck pain: a meta-analysis of randomized controlled trials. Spine. 2017 Jul 1;42(13):959-65. Link
19. Mathews JA. The effects of spinal traction. Physiotherapy. 1972 Feb;58(2):64-6.
20. Butler DS. The sensitive nervous system. Noigroup publications; 2000. Link
21. Diniz KT, Miranda RM, Ribeiro CD, Vasconcelos DA, Cabral-Filho JE. Neural mobilization effects in posterior myofascial chain flexibility and in head posture. Neurobiologia. 2010;73(3):53-7.
22. Grieve GP. Neck traction. Physiotherapy 1982;6:910-4.
23. Wong AM, Leong CP, Chen CM. The traction angle and cervical intervertebral separation. Spine. 1992 Feb;17(2):136-8. Link
24. Cervical Spine Stenosis and Myelopathy . The South African Spine Society. www.saspine.org/conditions/cer... spinal stenosis myelopathy.htm Retrieved from website 11/1/13
25. Zeller JL, Lynm C, Glass RM. Spinal stenosis. JAMA. 2008 Feb 27;299(8):980-. Link
26. Muthukumar N. Ossification of the ligamentum flavum as a result of fluorosis causing myelopathy: report of two cases. Neurosurgery. 2005 Mar 1;56(3):E622-. Link
27. Kumar VG, Rea GL, Mervis LJ, McGregor JM. Cervical spondylotic myelopathy: functional and radiographic long-term outcome after laminectomy and posterior fusion. Neurosurgery. 1999 Apr 1;44(4):771-7. Link
28. Kim HJ, Tetreault LA, Massicotte EM, Arnold PM, Skelly AC, Brodt ED, Riew KD. Differential diagnosis for cervical spondylotic myelopathy: literature review. Spine. 2013 Oct 15;38(22S):S78-88. Link
29. Clark CR, Benzel EC, Currier BL, et al. The Cervical Spine. Philadelphia, PA: Lippincott Williams & Wilkins; 2005.
30. Kasper D, Fauci A, Hauser S, Longo D, Jameson J, Loscalzo J. Harrison's principles of internal medicine. McGraw-Hill Professional Publishing; 2018.
31. Harris PR. Cervical traction: review of literature and treatment guidelines. Physical therapy. 1977 Aug 1;57(8):910-4. Link
32. Fritz JM, Thackeray A, Brennan GP, Childs JD. Exercise only, exercise with mechanical traction, or exercise with over-door traction for patients with cervical radiculopathy, with or without consideration of status on a previously described subgrouping rule: a randomized clinical trial. journal of orthopaedic & sports physical therapy. 2014 Feb;44(2):45-57. Link