Labral tears:

This article will focus on SLAP tears, which are one of the most common form of labral tear. Another common labral pathology is a Bankhardt lesion.
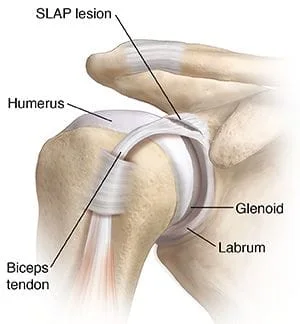
The acronym “SLAP” stands for Superior Labrum Anterior-Posterior, and is used to describe a tear or detachment of the shoulder’s labrum; generally originating at the anchor site for the long head of the biceps tendon and extending into anterior or posterior portions of the labrum. (1) This pathology is fairly common, in fact up to 1/4 of patients undergoing shoulder arthroscopy for any diagnosis will demonstrate a SLAP lesion (2,3). The labrum of the shoulder is a circumferential rim of fibrocartilage that surrounds the entire perimeter of the glenoid fossa (on the scapula) (4-6). The labrum shares some similar characteristics with the knee’s meniscus. (7) The inferior labrum is typically tightly attached to the bony glenoid rim, while the superior labrum is more “meniscus like” with a less secure union. (8)
The labrum serves as an attachment for tendons and ligaments and also deepens the glenoid fossa by 5-9 mm (4,10). Fifty percent of the glenoid depth is attributable to the labrum (11).
How do labral tears occur?
Labral tears may occur abruptly from injury or develop more slowly from repetitive microtrauma. (14) The forces associated with a labral injury typically include either superior compression or sudden inferior traction (14). Traumatic onsets, including a fall or direct blow to the shoulder, are responsible for almost 1/3 of all SLAP lesions. (14) The most common mechanism of acute injury involves a fall onto an outstretched arm. (14) SLAP lesions are common in athletic populations, particularly those requiring overhead motions that encourage the biceps to “pull” the labrum from its underlying bony attachment (1,15). In healthy shoulders, the long head of the biceps stabilizes the shoulder by generating compressive forces that limit translation, thereby, protecting the shoulde (16). The biceps also depresses the humeral head to protect the labrum and subacromial contents during arm lifting. Conversely, repetitive contraction of the biceps may trigger avulsion of its labral anchor – becoming progressively more problematic as the tear progresses (15). Chronic SLAP lesions do not typically occur in the absence of othershoulder problems; in fact, only 28% of SLAP tears are isolated problems (17). Chronic labrum issues are often associated with rotator cuff dysfunction. Weakened and irritated rotator cuff tendons lose their ability to hold the humeral head down within the glenoid cavity during arm lifting. Loss of this protective mechanism allows unchecked superior migration of the humeral head, and over time has the ability to “lift” the labrum from its attachment (14). Not surprisingly, a high percentage (29-45%) of patients with SLAP lesions also demonstrate rotator cuff pathology (17-19).
SLAP lesions commonly occur in young active males. (20) Throwers may be particularly vulnerable as this activity subjects the biceps tendon and its labral attachment to significant strain (15,21). A history of trauma or instability increases the likelihood of SLAP lesion (3,21). However, in many cases, patients present without a history of trauma or predisposing activity. (21)
Symptoms of SLAP lesions:
SLAP lesion complaints can vary from asymptomatic to disabling. Symptomatic patients often describe a deep, vague, non-specific shoulder pain that is provoked by overhead and cross-body activity (20,21). Weakness and stiffness often accompany the disorder. Discomfort may limit athletic performance, particularly in overhead athletes who may complain of a “dead arm” (20,21). Complaints of popping, clicking, grinding or catching are common (20,21) Patients with more advanced lesions are likely to report symptoms associated with instability; i.e. (pinching, slipping, apprehension or “looseness”- especially during overhead activity). The Biceps Load II Test has shown relatively high sensitivity and specificity in identifying isolated SLAP lesions. (26,34) The test is performed with the patient’s shoulder abducted to 120 degrees and externally rotated. The clinician stabilizes the patient’s arm while passively externally rotating until end range or patient apprehension. The patient then attempts to flex their elbow against the clinician’s resistance. An increase in pain suggests a SLAP lesion, while a decrease in apprehension or pain makes a SLAP lesion unlikely.
Is imaging necessary for a SLAP lesion?
Because the clinical assessment of SLAP lesion is difficult, imaging is the mainstay of diagnosis (41). X-rays cannot identify the presence of a SLAP lesion; however, these studies may be useful to rule out differential considerations, including degeneration, dislocation, fracture, or pathology. Diagnostic ultrasound is a useful modality for imaging SLAP tears with an added benefit of receiving patient feedback while evaluating their injury. MRI is typically included in the initial workup for patients with suspected labral pathology (42). MR arthrography provides the highest sensitivity and specificity for detecting SLAP lesions (42-47,61).
Moreover, the significance of a confirmed labral tear is debatable since this finding is present in more than half of asymptomatic, middle-aged patients (48) .
Treatment options for SLAP tears:
Conservative management of SLAP lesions is frequently unsuccessful. (49-51). However, the presence of a SLAP lesion does not automatically necessitate surgical intervention. However, the imaged defect is not necessarily the primary contributor to the patient’s complaint. Most experts, including the American Academy of Orthopedic Surgeons, recommends a 6-12 week course of conservative management prior to considering surgical intervention (50-52). Non-surgical treatment correcting scapular dyskinesis and deficits in internal rotation has a reasonable success rate in MLB players with a documented SLAP lesion (64). Conservative treatment goals include pain reduction, enhancing mobility, and restoration of strength (51). Initial management includes anti-inflammatory medications/ modalities and cessation of provocative activities (i.e. throwing) (51). Flexibility programs are incorporated as symptoms allow.
Progressive strengthening of the scapular and rotator cuff musculature is implemented as tolerated. Strengthening exercises should focus on re-balancing strength between anterior (pec, upper traps) and posterior muscle groups (lower traps, serratus anterior, rhomboid).
Rehabilitation must restore serratus anterior strength and proper scapular function- thoroughly addressing regional biomechanical deficits including scapular dyskinesis and upper crossed syndrome, as well as more distant sites of dysfunction including the hip and trunk. Myofascial release may be directed at the subscapularis, infraspinatus, anterior shoulder musculature and the posterior capsule (53). Manipulation may be helpful to restore mobility to restricted cervical or thoracic segments.
Only 7-57% of elite overhead athletes are able to return to pre-injury level of competition following surgical SLAP repair. (63,64) The co-existence of a partial-thickness rotator cuff tear correlates with inability to return to this level of competition (63) Surgeons may elect to perform debridement, suturing, or excision based upon the type of lesion (54). Surgical intervention should address concurrent shoulder pathology; i.e. rotator cuff lesions, degeneration, instability, etc. (54). Surgical repair typically entails a four to six-month post-operative rehab (55).
At Creekside Chiropractic & Performance Center, we are highly trained to treat this condition. We are the only inter-disciplinary clinic in Sheboygan county that provides chiropractic, myofascial release, ART (Active Release Technique), massage therapy, acupuncture, physiotherapy, rehabilitative exercise, nutritional counseling, personal training, and golf performance training under one roof. Utilizing these different services, we can help patients and clients reach the best outcomes and the best versions of themselves. Voted Best Chiropractor in Sheboygan by the Sheboygan Press.
Evidence Based-Patient Centered-Outcome Focused
Sources:
1. Knesek M, Skendzel JG, Dines JS, et al. Diagnosis and management of superior labral anterior posterior tears in throwing athletes. Am J Sports Med 2013;41(2): 444–60.
2. Kim TK, Queale WS, Cosgarea AJ, McFarland EG. Clinical features of the different types of SLAP lesions: an analysis of one hundred and thirty-nine cases. J Bone Joint Surg Am. 2003 Jan. 85-A(1):66-71.
3. Kampa RJ, Clasper J. Incidence of SLAP lesions in a military population. J R Army Med Corps. 2005 Sep. 151(3):171-5.
4. Snyder SJ, Karzel RP, Del Pizzo W, Ferkel RD, Friedman MJ. SLAP lesions of the shoulder. Arthroscopy. 1990. 6(4):274-9.
5. Moseley H, Overgaard B. The anterior capsular mechanism in recurrent anterior dislocation of the shoulder. Morphological and clinical studies with special reference to the glenoid labrum and glenohumeral ligaments. J Bone Joint Surg Br. 1962. 44B:913-27.
6. Detrisac DA, Johnson LL. Arthroscopic Shoulder Anatomy: Pathological and Surgical Implications. Thorofare, NJ: Slack Inc; 1986.
7. Soslowsky LJ, Flatow EL, Bigliani LU, et al. Quantitation of in situ contact areas at the glenohumeral joint: a biomechanical study. J Orthop Res 1992;10(4):524–34
8. Williams RJ. Superior Labrum Tears. Medscape. http://emedicine.medscape.com/article/92512-overview#a5. Accessed Feb 12, 2016.
9. Vangsness CT Jr, Jorgenson SS, Watson T, Johnson DL. The origin of the long head of the biceps from the scapula and glenoid labrum. An anatomical study of 100 shoulders. J Bone Joint Surg Br. 1994 Nov. 76(6):951-4.
10. Rockwood CA, Matsen FA, Wirth MA. The shoulder, vol. 1. Philadelphia: WB Saunders; 2009.
11. Howell SM, Galinat BJ. The glenoid-labral socket. A constrained articular surface. Clin Orthop Relat Res 1989;(243):122–5.
12. Williams RJ. Superior Labrum Tears. Medscape. http://emedicine.medscape.com/article/92512-overview#a5. Accessed Feb 12, 2016.
13. Prodromos CC, Ferry JA, Schiller AL, Zarins B. Histological studies of the glenoid labrum from fetal life to old age. J Bone Joint Surg Am. 1990 Oct. 72(9):1344-8.
14. Dessaur WA. (2008). Diagnostic Accuracy of Clinical Testing for Superior Labral Anterior Posterior Lesions: A Systematic Review Journal of Orthopaedic and Sports
15. Andrews JR, Carson WG Jr, McLeod WD. Glenoid labrum tears related to the long head of the biceps. Am J Sports Med. 1985 Sep-Oct. 13(5):337-41.
16. Pagnani MJ, Deng XH, Warren RF, Torzilli PA, Altchek DW. Effect of lesions of the superior portion of the glenoid labrum on glenohumeral translation. J Bone Joint Surg Am. 1995 Jul. 77(7):1003-10.
17. Snyder SJ, Banas MP, Karzel RP: An analysis of 140 injuries to the superior glenoid labrum. J Shoulder Elbow Surg 4: 243-248, 1995.
18. Andrews JR, Carson WG. The arthroscopic treatment of glenoid labrum tears in the throwing athlete. Orthop Trans. 1984;8:44.
19. Mileski RA, Snyder SJ. Superior labral lesions in the shoulder: pathoanatomy and surgical management. J Am Acad Orthop Surg. 1998;6:121–131
20. David A. Cortese and Stephen J. Snyder Superior Labral Anterior-Posterior Lesions of the Shoulder THE ATHLETE’S SHOULDER (Second Edition), 2009, Pages 269-282
21. Bedi A, Allen AA. Superior labral lesions anterior to posterior-evaluation and
arthroscopic management. Clin Sports Med 2008;27(4):607–30.
22. Gabel CP, Yelland M, Melloh M, et al. A modified QuickDASH-9 provides a valid outcome instrument for upper limb function. BMC Musculoskelet Disord 2009;10:161.
23. Roy JS, MacDermid JC, Woodhouse LJ. Measuring shoulder function: a system- atic review of four questionnaires. Arthritis Rheum 2009;61(5):623–32.
24. Godfrey J, Hamman R, Lowenstein S, et al. Reliability, validity, and responsive- ness of the simple shoulder test: psychometric properties by age and injury type. J Shoulder Elbow Surg 2007;16(3):260–7.
25. MacDermid JC, Solomon P, Prkachin K. The shoulder pain and disability index demonstrates factor, construct and longitudinal validity. BMC Musculoskelet Dis- ord 2006;7:12.
26. Cook C et al. Diagnostic accuracy of five orthopedic clinical tests for diagnosis of superior labrum anterior posterior (SLAP) lesions Journal of Shoulder and Elbow Surgery. Vol 21, Issue 1 January 2012, Pages 13–22
27. Guanche CA, Jones DC: Clinical testing for tears of the glenoid labrum. Arthroscopy 19:517-523, 2003.
28. Holtby R, Razmjou B: Accuracy of the Speed’s and Yergason’s tests in detecting biceps pathology and SLAP lesions: Comparison with arthroscopic findings. Arthroscopy. 20:231-236, 2004.
29. McFarland EG, Kim TK, Savino RM: Clinical assessment of three common tests for superior labral anterior-posterior lesions. Am J Sports Med 30:810-815, 2002.
30. Dutton Mark. Orthopaedic examination, evaluation, and intervention. New York: McGraw Hill; 2004.
31. Dessaur WA. (2008). Diagnostic Accuracy of Clinical Testing for Superior Labral Anterior Posterior Lesions: A Systematic Review Journal of Orthopaedic and Sports
32. Stetson WB, Templin K. The crank test, the O'Brien test, and routine magnetic resonance imaging scans in the diagnosis of labral tears. Am J Sports Med. 2002;30:806–809.
33. Yang-Soo Kim, Jung-Man Ha, Kee Yong, et al. The passive compression test: A new clinical test for superior labral tears of the shoulder. Am J Sports Med, 2007;35(9):1489-94.
34. Kim SH et al. Biceps Load Test II: A Clinical test for SLAP lesions of the Shoulder. Arthroscopy 2001
35. O'Brien SJ, Pagnani MJ, Fealy S, McGlynn SR, Wilson JB. The active compression test: a new and effective test for diagnosing labral tears and acromioclavicular joint abnormality. Am J Sports Med. 1998;26:610–613
36. Dodson CC, Altchek DW. SLAP Lesions: An Update on Recognition and Treatment. JOSPT February 2009, Volume 39 Number 2
37. Dessaur WA. (2008). Diagnostic Accuracy of Clinical Testing for Superior Labral Anterior Posterior Lesions: A Systematic Review Journal of Orthopaedic and Sports
38. Snyder SJ, Karzel RR, Del Pizzo W, Ferkel RD, Friedman MJ. SLAP lesions of the shoulder. Arthroscopy. 1990;6:274–279
40. Myers TH, Zemanovic JR, Andrews JR. The resisted supination external rotation test: a new test for the diagnosis of superior labral anterior posterior lesions. Am J Sports Med. 2005;33:1315–1320.
41. George D. Chloros et al., Imaging of Glenoid Labrum Lesions Clin Sports Med 32 (2013) 361–390
42. Williams RJ. Superior Labrum Tears. Medscape. http://emedicine.medscape.com/article/92512-overview#a5. Accessed Feb 12, 2016.
43. Fallahi F, Green N, Gadde S, Jeavons L, Armstrong P, Jonker L. Indirect magnetic resonance arthrography of the shoulder; a reliable diagnostic tool for investigation of suspected labral pathology. Skeletal Radiol. 2013 Sep. 42(9):1225-33.
44. Modi CS, Karthikeyan S, Marks A, Saithna A, Smith CD, Rai SB, et al. Accuracy of abduction-external rotation MRA versus standard MRA in the diagnosis of intra-articular shoulder pathology. Orthopedics. 2013 Mar. 36(3):e337-42.
45. Magee T, Williams D, Mani N. Shoulder MR arthrography: which patient group
benefits most? AJR Am J Roentgenol 2004;183(4):969–74.
46. Monu JU, Pope TL Jr, Chabon SJ, Vanarthos WJ. MR diagnosis of superior labral anterior posterior (SLAP) injuries of the glenoid labrum: value of routine imaging without intraarticular injection of contrast material. AJR Am J Roentgenol. 1994 Dec. 163(6):1425-9.
47. Waldt S, Burkart A, Lange P, et al. Diagnostic performance of MR arthrography in the assessment of superior labral anteroposterior lesions of the shoulder. AJR Am J Roentgenol. 2004 May. 182(5):1271-8.
48. Schwartzberg R, Reuss BL, Burkhart BG et al. High Prevalence of Superior Labral Tears Diagnosed by MRI in Middle-Aged Patients With Asymptomatic Shoulders. Journal of Sports Medicine. January 2016 vol. 4 no. 1
49. Williams RJ. Superior Labrum Tears. Medscape. http://emedicine.medscape.com/article/92512-treatment. Accessed Feb 12, 2016
50. Mileski RA, Snyder SJ. Superior labral lesions in the shoulder: pathoanatomy and surgical management. J Am Acad Orthop Surg. 1998 Mar-Apr. 6(2):121-31
51. Dodson CC, Altchek DW. SLAP Lesions: An Update on Recognition and Treatment. JOSPT February 2009, Volume 39 Number 2
52. Franceschi F, Longo UG, Ruzzini L, et al. No advantages in repairing a type II su- perior labrum anterior and posterior (SLAP) lesion when associated with rotator cuff repair in patients over age 50: a randomized controlled trial. Am J Sports Med 2008;36(2):247–53.
53. Hammer W. Conservative Treatment of SLAP Tears. Dynamic Chiropractic. September 9, 2010, Vol. 28, Issue 19
54. Huang H, Zheng X, Li P, Shen H. Arthroscopic reconstruction of shoulder's labrum with extensive tears. Int J Surg. 2013. 11(9):876-81
55. Williams RJ. Superior Labrum Lesions. Medscape http://emedicine.medscape.com/... accessed 8.11.15
57. Wilk KE, Reinold MM, Dugas JR, Arrigo CA, Moser MW, Andrews JR. Current concepts in the recognition and treatment of superior labral (SLAP) lesions. J Orthop Sports Phys Ther. 2005;35:273–291.
58. Tirman PF, Applegate GR, Flannigan BD, Stauffer AE, Crues JV. Magnetic resonance arthrography of the shoulder. Magn Reson Imaging Clin N Am 1993; 1:125–142
59. Waldt S, Metz S, Burkart A, et al. Variants of the superior labrum and labro-bicipital complex: a comparative study of shoulder specimens using MR arthrography, multi-slice CT arthrography and anatomical dissection. Eur Radiol 2006; 16:451–458
60. Tirman PF, Bost FW, Steinbach LS, et al. MR arthrographic depiction of tears of the rotator cuff: benefit of abduction and external rotation of the arm. Radiology 1994; 192:851–856
61. Tuite MJ, et al. Imaging Evaluation of Nonacute Shoulder Pain. AJR Am J Roentgenol. 2017 May 24:1-9. doi: 10.2214/AJR.17.18085. [Epub ahead of print]
62. Laughlin WA, et al. Deficiencies in pitching biomechanics in baseball players with a history of superior labrum anterior-posterior repair. Am J Sports Med. 2014. Dec;42(12):2837-41.
63. Neri BR, et al. Outcome of type II superior labral anterior posterior repairs in elite overhead athletes: Effect of concomitant partial-thickness rotator cuff tears. Am J Sports Med. 2011 Jan;39(1):114-20. Epub 2010 Oct 12.
64. Fedoriw WW, et al. Return to play after treatment of superior labral tears in professional baseball players. Am J Sports Med. 2014. May;42(5):1155-60. Epub 2014 Mar 27.
