What is patellofemoral pain syndrome?
Patellofemoral pain syndrome (PFPS), also called "Runners Knee", describes the symptom grouping of knee discomfort, swelling or clicking that is caused by excessive and/or imbalanced forces on the knee joint. The broad term “Patellofemoral pain syndrome” (PFPS) is a spectrum of signs and symptoms. The spectrum begins with non-painful functional mis-alignment of the knee cap and ends in severe patellofemoral arthritis.
How common is PFPS?
It is the most common cause of knee pain in the general population, affecting an estimated 25% of adults (1,5,23). Many PFPS patients are young and athletic (32). Data suggests the condition may affect nearly 10% of young athletes (2).
What causes patellofemoral pain syndrome?
PFPS is most common from muscular imbalance and cumulative overload. The issues typically begin as imbalances between the knee stabilizing muscles, which changes the forces on the patella (knee cap) and the surrounding tissues (cartilage). These stressors are compounded through activities of daily living, causing irritation and eventually wear to the patellofemoral cartilage.
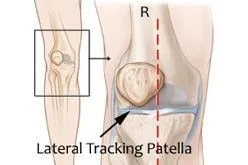
PFPS is most commonly related to lateral tracking of the patella (4). The patella has a natural tendency to migrate laterally due to the pull of the quadriceps and the natural positioning of the hips, knees, ankles, and feet (5).
Compounding this problem it the fact that the patellofemoral orientation is largely determined by the hip and foot (6,7,40). Pes planus (flat feet) or over pronation causes internal rotation of the tibia and knee, placing stress on the lateral aspect of the knee cartilage- increasing one's risk of PFPS (8,24,40). Gluteus medius (Hip Abductor) weakness is associated with inward flare of the knee (knock knees) and lateral tracking of the kneecap (40-44). Current research suggests that patellar movement and tracking is more dependent on femur and tibia biomechanics than any individual knee muscle strength (26,40).
What are the symptoms of Patellofemoral Pain Syndrome?
PFPS patients generally present with dull pain around the kneecap that is worse with activites that load the joint, including prolonged walking, running, squatting, jumping, kneeling, arising from a seated position or stair climbing- especially walking down stairs or downhill. Swelling may accompany the pain. Damage of patellofemoral cartilage may result in clicking, intermittent locking, or giving way (27).
What are the risk factors for patellofemoral pain syndrome?
Risk factors include joint overload/ overuse, trauma, tight lateral knee capsule, excess movement of the patella, and muscular imbalance- particularly quadriceps or iliotibial band tightness and quadriceps weakness (9,28-30). Weakness in the quadriceps or hamstring muscles increases one’s risk of developing the problem three to five times more likely (24). Gluteal weakness is common and may contribute (12,33).
What are the best treatment options for patellofemoral pain?
Best practice guidelines suggest implementing exercise, bracing, foot orthoses and combined interventions of manual therapy and SMT (51,52).
Early management begins with avoiding aggravating factors and decreasing inflammation and transitions to long term correction of functional deficits (30). Reducing pain-provoking activities is an early priority, especially running, jumping and activities that induce a knock-knee position. Athletes should avoid allowing their knee to cross in front of their toes while squatting.
Electrotherapy and ice may be useful early on for reduction of pain and inflammation.
Myofascial release and stretching should be directed at hypertonic muscles.
Combining manual therapy with physical therapy reduces pain and improves function, especially when strengthening both hip and knee muscles (39). Exercise has a positive effect on PFPS patients, especially Gluteus medius and VMO (19, 40, 45-49). Eccentric exercises are also more effective than concentric.
Manipulation may be necessary for restrictions in the lumbosacral and lower extremity joints.
Taping the area may not address the source of the problem (20,21) yet, clinical practice guidelines do utilize corrective taping (51,52). Patellar tracking braces (i.e. BioSkin or PatellaPro) may lead to better outcomes (50-52).
Arch supports or custom orthotics may be necessary to correct hyperpronation (40). Research has shown that runners with PFPS benefit from a combination of exercise and foot orthotics (22). Runners should change shoes about every 250 miles.
At Creekside Chiropractic & Performance Center, we are highly trained to treat this condition. We are the only inter-disciplinary clinic providing services to Sheboygan, Sheboygan Falls, Plymouth, and Oostburg including chiropractic, manual therapy, myofascial release, ART (Active Release Technique), massage therapy, acupuncture, physiotherapy, rehabilitative exercise, nutritional counseling, personal training, and golf performance training under one roof. Utilizing these different services, we can help patients and clients reach the best outcomes and the best versions of themselves. Voted Best Chiropractor in Sheboygan by the Sheboygan Press.
Evidence Based-Patient Centered-Outcome Focused
Sources:
1. Baquie P, Brukner P. Injuries presenting to an Australian sports medicine centre: a 12-month study. Clin J Sport Med. 1997;7:28-31.
2. Myer GD, Ford KR, Barber Foss KD, et al. The incidence and potential pathomechanics of patellofemoral pain in female athletes. Clin Biomech (Bristol, Avon) 2010; 25:700–7.
3. Reilly DT, Martens M. Experimental analysis of the quadriceps muscle force and patellofemoral joint reaction force for various activities. Acta Orthop Scand. 1972;43:126–37.
4. Doucette SA, Goble EM. The effect of exercise on patellar tracking in lateral patellar compression syndrome. Am J Sports Med. 1992;20:434-440.
5. Wilson T, The Measurement of Patellar Alignment in Patellofemoral Pain Syndrome: Are We Confusing Assumptions With Evidence? JOSPT June 2007, Vol 37, Number 6
6. Griffin LY, Agel J, Alborhm MJ, et al. Non-contact anterior cruciate ligament injuries: risk factors and prevention strategies. J Am Acad Orthop Surg, 2000;8:141-50
7. Bobbert MF, van Zandwijk JP. Dynamics of force and muscle stimulation in human vertical jumping. Med Sci Sports Exerc, 1999;31:303-10
8. Zappala FG, Taffel CB, Scuderi GR. Rehabilitation of patellofemoral joint disorders. Orthop Clin North Am. 1992;23:555–66.
9. Puniello MS. Iliotibial band tightness and medial patellar glide in patients with patellofemoral dysfunction. J Orthop Sports Phys Ther. 1993;17:144–8.
10. Liebenson C. Functional problems associated with the knee—Part one: Sources of biomechanical overload Journal of Bodywork and Movement Therapies (2006) 10, 306–311
12. Ireland ML, Willson JD, Ballantyne BT, McClay-Davis I. Hip strength in females with and without patellofemoral pain. J Orthop Sports Phys Ther, 2004;33:671-6.
13. Fitzgerald GK, McClure PW. Reliability of measurements obtained with four tests for patello--femoral alignment. Phys Ther. 1995;75:84-92
14. Watson CJ, Propps M, Galt W, Redding A, Dobbs D. Reliability of McConnell’s classification of patellar orientation in symptomatic and asymptomatic subjects. J Orthop Sports Phys Ther. 1999;29:378-385; discussion 386-393
15. Tomsich DA, Nitz AJ, Threlkeld AJ, Shapiro R. Patellofemoral alignment: reliability. J Orthop Sports Phys Ther. 1996;23:200–8.
16. Reid DC. Sports injury assessment and rehabilitation. New York: Churchill Livingstone, 1992:345–98.
17. Dixit S, Difiori JP. Management of Patellofemoral Pain Syndrome. Am Fam Physician. 2007 Jan 15;75(2):194-202.
18. Calmbach WL, Hutchens M. Evaluation of patients presenting with knee pain: Part II. Diferential diagnosis Am Family Phys 2003. Sept 1;68(5) 917-922
19. Powers CM. The influence of altered lower-extremity kinematics on patellofemoral joint dysfunction: a theoretical perspective. J Orthop Sports Phys Ther, 2003;33:639-46
20. Warden S J, Hinman RS, Watson MA Jr, et al. Patellar taping and bracing for the treatment of chronic knee pain: a systematic review and meta- analysis. Arthritis Rheum 2008; 59:73–83.
21. McConnell JS. The management of chondromalacia patellae: a long-term solution. Aust J Physiotherapy. 1986;32:215–23.
22. Eng JJ, Pierrynowski MR. Evaluation of soft foot orthotics in the treatment of patellofemoral pain syndrome. Phys Ther 1993; 73:62–8; discussion 68–70
23. Tobin S, Robinson G. The effect of McConnell’s vastus lateralis inhibition taping technique on vastus lateralis and vastus medialis obliquus activity. Physiotherapy. 2000;86:173-183.
24. Boling MC, Padua DA, Marshall SW, et al. A Prospective Investigation of Biomechanical Risk Factors for Patellofemoral Pain Syndrome. Am J Sports Med November 2009 vol. 37 no. 11 2108-2116
25. Ashraf Ramadan Hafez, Abdulrahim Zakaria and Syamala Buragadda, Eccentric versus Concentric Contraction of Quadriceps Muscles in Treatment of Chondromalacia Patellae World Journal of Medical Sciences 7 (3): 197-203, 2012
26. Sawatsky A et. al, Changes in patellofemoral joint contact pressures caused by vastus medialis muscle weakness Clinical Biomechanics 27 (2012) 595–601
27. Thomee R, Augustsson J, Karlsson J. Patellofemoral pain syndrome: a review of current issues. Sports Med 1999;28:245-62.
28. Waryasz GR, McDermott AY. Patellofemoral pain syndrome (PFPS): a systematic review of anatomy and potential risk factors. Dynamic Medicine. 2008, 7:9. doi:10.1186/1476-5918-7-9.
29. Lankhorst NE, Bierma-Zeinstra SMA, Middelkoop MV. Risk Factors for Patellofemoral Pain Syndrome: A Systematic Review. J Orthop Sports Phys Ther. Epub 25 October 2011. Doi: 10.2519/jospt 2012.3803.
30. Piva SR, Fitzgerald GK, Wisniewski S, Delitto A. Predictors of pain and function outcome after rehabilitation in patients with patellofemoral pain syndrome. J Rehabil Med. 2009; 41(8): 604–612. doi: 10.2340/16501977-0372.
31. Huberti HH, Hayes WC. Patellofemoral contact pressures. The influence of q-angle and tendofemoral contact. J Bone Joint Surg Am. Jun 1984;66(5):715-24.
32. Dixit S, Burton M, Mines B. Management of Patellofemoral Pain Syndrome. Am Fam Physician. 2007 Jan 15;75(2):194-202.
33. Bolgla LA, Malone TR, Umberger BR, Uhl TL. Hip Strength and Hip and Knee Kinematics During Stair Descent in Females With and Without Patellofemoral Pain Syndrome. J Orthop Sports Phys Ther. 2008;38(1):12-18. doi:10.2519/jospt.2008.2462.
34. Abernethy P, Wilson G, Logan P. Strength and power assessment. Issues, controversies and challenges. Sports Med 1995;19:401-17.
35. Scott T Doberstein, MS, LAT, ATC, CSCS, Richard L Romeyn, MD, and David M Reineke, PhD The Diagnostic Value of the Clarke Sign in Assessing Chondromalacia Patella J Athl Train. 2008 Mar-Apr; 43(2): 190–196.
36. Cook C, Mabry L, Reiman M, Hegedus E. Best tests/clinical findings for screening and diagnosis of patellofemoral pain syndrome: a systematic review Physiother. 2011,
37. M S Rathleff, C R Rathleff, K M Crossley, C J Barton Is Hip Strength a Risk Factor for Patellofemoral Pain? A Systematic Review and Meta- analysis Br J Sports Med. 2014;48(14):1088
38. Brown, Courtney K. et al. The Effectiveness of Exercise on Recovery and Clinical Outcomes in Patients With Soft Tissue Injuries of the Hip, Thigh, or Knee: A Systematic Review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Journal of Manipulative & Physiological Therapeutics , Volume 39 , Issue 2 , 110 - 120.e1
39. Espí-López, Gemma Victoria et al. Effectiveness of Manual Therapy Combined With Physical Therapy in Treatment of Patellofemoral Pain Syndrome: Systematic Review Journal of Chiropractic Medicine , Volume 16 , Issue 2 , 139 – 146
40. Petersen W, Rembitzki I, Liebau C. Patellofemoral pain in athletes. Open Access Journal of Sports Medicine. 2017;8:143-154.
41. Baldon Rde M, Nakagawa TH, Muniz TB, Amorim CF, Maciel CD, Serrão FV. Eccentric hip muscle function in females with and without patellofemoral pain syndrome. J Athl Train. 2009;44(5):490–496.
42. Bolgla LA, Malone TR, Umberger BR, Uhl TL. Hip strength and hip and knee kinematics during stair descent in females with and without patellofemoral pain syndrome. J Orthop Sports Phys Ther. 2008;38(1):12–16.
43. Brent JL, Myer GD, Ford KR, Hewett TE. A longitudinal examination of hip abduction strength in adolescent males and females. Med Sci Sports Exerc. 2008;39:34–45.
44. Prins MR, van der Wurff P. Females with patellofemoral pain syndrome have weak hip muscles: a systematic review. Aust J Physiother. 2009;55(1):9–15.
45. Harvie D, O’Leary T, Kumar S. A systematic review of randomized controlled trials on exercise parameters in the treatment of patellofemoral pain: what works? J Multidiscip Healthc. 2011;4:383–392.
46. Alba-Martín P, Gallego-Izquierdo T, Plaza-Manzano G, Romero-Franco N, Núñez-Nagy S, Pecos-Martín D. Effectiveness of therapeutic physical exercise in the treatment of patellofemoral pain syndrome: a systematic review. J Phys Ther Sci. 2015;27(7):2387–2390.
47. Peters JS, Tyson NL. Proximal exercises are effective in treating patellofemoral pain syndrome: a systematic review. Int J Sports Phys Ther. 2013;8(5):689–700.
48. Thomson C, Krouwel O, Kuisma R, Hebron C. The outcome of hip exercise in patellofemoral pain: a systematic review. Man Ther. 2016;26:1– 30.
49. van der Heijden RA, Lankhorst NE, van Linschoten R, Bierma-Zeinstra SM, van Middelkoop M. Exercise for treating patellofemoral pain syndrome. Cochrane Database Syst Rev. 2015;1:CD010387.
50. Petersen W, Ellermann A, Rembitzki IV, et al. Evaluating the potential synergistic benefit of a realignment brace on patients receiving exercise therapy for patellofemoral pain syndrome: a randomized clinical trial. Arch Orthop Trauma Surg. 2016;136(7):975–982.
51. Barton CJ, Lack S, Hemmings S, Tufail S, Morrissey D. The ‘Best Practice Guide to Conservative Management of Patellofemoral Pain’: incorporating level 1 evidence with expert clinical reasoning. Br J Sports Med. 2015;49(14):923–923.
52. Crossley KM, van Middelkoop M, Callaghan MJ, et al. Patellofemoral pain consensus statement from the 4th International Patellofemoral Pain Research Retreat, Manchester. Part 2: recommended physical interventions (exercise, taping, bracing, foot orthoses and combined interventions) Br J Sports Med. 2016;50(14):844–852.
53. Fox A, Ferber R, Saunders N, Osis S, Bonacci. Gait Kinematics in Individuals with Acute and Chronic Patellofemoral Pain. J. Med Sci Sports Exerc. 2018 Mar;50(3):502-509